Diving Into The World Of HBOT
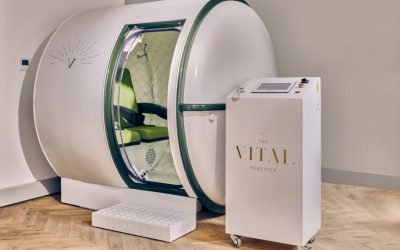
Get the latest news and research on Hyperbaric Oxygen Therapy, also known as HBOT. Hyperbaric Oxygen Therapy involves breathing 100% oxygen under pressure while in a hyperbaric chamber, and is used to treat an extensive list of conditions involving tissue damage and inflammation.
Subscribe below to receive updates on the latest HBOT related news & research, as well as personal interviews & stories from researchers, practitioners, and patients who’ve found hope in HBOT. Stay tuned as we dive into the phenomenon that is Hyperbaric Oxygen Therapy.
Listen to or Watch the HBOT Conversations Podcast
Listen to the HBOT Converstations podcast by downloading it from your favorite podcasting platform or watch an episode here on the HBOT News:
Special Report – A Medical Revolution
Explore the profound benefits of HBOT in treating various health conditions, focusing on its anti-inflammatory and healing properties.
Recent News & Research
HBOT Helps Cancer Patients Heal Faster
Radiation can not only kill the tumor, but also the healthy surrounding tissue. Because of this, cancer patients often find that healing from radiation treatments is complicated and painful. Thankfully, Hyperbaric Oxygen Therapy is helping cancer...
How hyperbaric oxygen treatment (HBOT) may help cancer patients
Could HBOT help someone eliminate cancer from their bodies? Amberin Fur, who goop by Gweneth Paltrow (a homespun weekly newsletter) labeled as London’s best osteopath, seems to think so. It made a world of difference in her mother. When osteopath...
Nevada Legislature bill would urge study into hyperbaric oxygen therapy for veterans
Hyperbaric oxygen chamber (Healing with Hyperbarics North Dakota) By Michael Bell Published: Mar. 15, 2023 at 4:56 PM EDT LAS VEGAS, Nev. (FOX5) - If passed, a bill in the Nevada Legislature would urge the U.S. Department of Veterans Affairs to...
HBOT at HCMC Saved 2-Year Old’s Ear After Dog Bite
Image Credits: FAMILY IMAGE PROVIDED FOR STAR TRIBUNE When two-year old, Kenize was bitten by a puppy in a freak accident, she easily could have lost the top 1/3 of her ear. Yet, it was Hyperbaric Oxygen Therapy that saved the day; and her ear....
HBOT Protocol very effective for Fibromyalgia caused by TBI
Researchers from Tel Aviv University compared treatment with a dedicated protocol of hyperbaric oxygen therapy (HBOT) to the pharmacology (drugs) treatment available today for patients suffering from fibromyalgia as a result of a traumatic brain...
A Veteran’s HBOT Success Story for PTSD & Long-COVID
This veteran, John Ahlers, has been doing HBOT dives at Des Moines HBOT Center under the care of Dr. Vince Hassel for the past month. His interest in HBOT started as a way to help Long-COVID, but as a veteran suffering from PTSD he is now seeing...
New HBOT Facility in Rugby makes Headline News
Karina and Mac Dragon brought a new HBOT facility to the UK by recently opening O2 Hyper Health in Rugby. Karina said the treatment's benefits are endless and can help with health and beauty issues. "Our mission is to help our community live and...
HBOT Makes List of Top 10 Reasons to Visit Newport Beach
Newport Beach in California has earned a reputation to be a bit of a playground for the upper class, while providing access to the most state-of-the art options for health & wellness. It's no surprise that HBOT was included in Luxury Lifestyle...
Why Combat Veterans Are Turning to Oxygen Therapy for PTSD
IMAGE: "Army Sgt. Margaux Mange experienced severe PTSD symptoms after serving in Iraq. She says hyperbaric oxygen therapy helped her symptoms significantly improve". Visual: Courtesy Margaux Mange via UNDARK.ORGHyperbaric Oxygen Therapy has been...